Rhawn Gabriel Joseph, Ph.D.
BrainMind.com
FUNCTIONAL NEUROANATOMY OF PARIETAL AREA 5
Parietal Area 7
The parietal lobes are not a homologous tissue but consists of cells which are responsive to a variety of divergent stimuli, including movement, hand position, objects within grasping distance, audition, eye movement, pain, heat, cold, as well as complex and motivationally significant visual stimuli (Aoki et al., 1999; Cohen et al. 2014; Deibert et al., 1999; Dong et al. 2014; Lam, et al., 1999; Lebedev et al. 2014; Lin & Sessle 2014; Pred'Homme & Kalaska 2014; Remy et al., 1999; Snyder et al., 1998).
For example, area 7 of the superior parietal lobe receives considerable visual input, particularly from the lower visual fields and periphery--information which it receives not only from the visual cortex but from extra-retinal pathway. Area 7 also receives complex somesthetic stimuli regarding the hand and objects beyond and within reaching distance. Moreover, different neurons in different regions of area 7 perform somewhat different functions. Even the subareas within the primary somesthetic neocortex, areas 3ab,1, 2, respond to different stimuli and receive projections from different subregions within the thalamus, which in turn receive different forms of input from skin, joints and muscles.
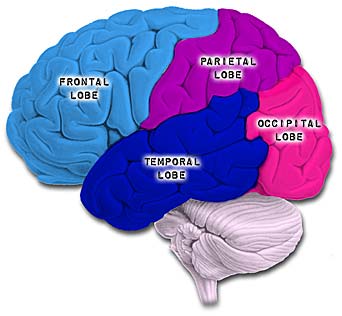
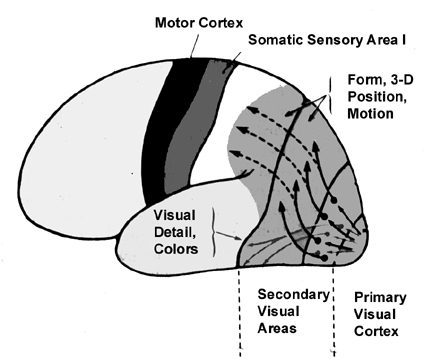

Because it serves so many diverse yet related functions, damage to the parietal lobe can therefore result in a variety of disturbances. This includes abnormalities involving somesthetic and pain sensation, the body image, visual-spatial relations, temporal-sequential motor activity, language, grammar, numerical calculation, emotion, and attention, depending on which area has been lesioned as well as the laterality of the damage.
PARIETAL TOPOGRAPHY
There are nine major somesthetic areas within the parietal lobe, such that the primary, association, and assimilation areas actually consist of numerous subareas. Broadly, and most generally, however, the parietal lobe may be subdivided into a primary receiving area (involving Brodmann's areas 3ab,1,2) within the post central gyrus, an immediately adjacent somesthetic association area (Brodmann's area 5ab), a polymodal (visual, motor, somesthetic) receiving area located in the superior-posterior parietal lobule (area 7ab), a granular insular area which is located in the inferior convexity and encompasses part of the marginal gyrus, and a multimodal-assimilation area within the inferior parietal lobule (areas 7, 39, 40) which encompasses the angular and supramarginal gyrus.

THE SOMESTHETIC (SUPPLEMENTARY) ASSOCIATION AREA
Neurons in area 5 receive information already analyzed in the immediately adjacent primary somesthetic cortices, some cells in the association area (Brodmann's area 5ab) also receive input from the contrateral primary zone (via the corpus callosum) as well as from the motor association areas (area 6) in the frontal lobes (Dong et al. 2014; Jones & Powell, 1970) and from subdivision within the thalamus the posterior ventral posterior complex (Burton, 2016; Friedman & Murray, 2016; Kaas, 1993). Due in large part to the callosal interconnections, both halves of the body, the trunkal area in particular (Robinson, 2015) come to be represented in this region. Indeed, the two halves of the body appear to be superimposed such that the body is bilaterally represented (Whitsel et al. 1969).
However, as based on behavioral and electrophysiological data from intact and brain damaged individuals, bilateral represention is predominantly maintained within the right half of the human brain. It is this greater and bilateral degree of representation and the more unilateral nature of left parietal representation, which explains the greater incidence of neglect (see below) and the greater degree of hemiplegia and hemianesthesia which is seen after right vs left parietal lesions (Sterzi et al., 1993).





HAND MANIPULATION CELLS
A small percentage of cells in area 5 also appear to be concerned with more complex activities such as the movement of the hand and arm and the manipulation of objects (Cohen et al. 2014; Mountcastle et al., 2015). Indeed, a detailed representation of the cutaneous surface of the body, and in particular, the hand (and face), is maintained in here (Burton, et al. 1982; Lin et al. 2014). These are referred to as "hand-manipulation cells". In fact, electrical stimulation of area 5 can result in limb movements (Hyvariene, 1982) whereas experimentally induced tactile extinction of either the right or left hand can induce bilateral reductions in activity in this region (Remy et al., 1999).
In consequence, injury to this part of the brain can interfere with hand movements. For example, a patient I examined with a right superior parietal tumor, was unable, both before and after surgery, to correctly reach for items that were located to the left or right side of his body and would invariable miss or knock the items over. He displayed stereognosis when he was asked to name (with his eyes closed) objects held in his right or left hand (worse in the left hand) also had severe difficulty with block design and puzzles from the WAIS-R, could not throw or catch with accuracy, and suffered a loss of vision in the left lower quadrant of his visual field--though there was no evidence of neglect. In fact, according to this patient, the first sign of his illness was the loss of the ability to throw with accuracy, which he noticed when he began missing the "basket ball" hoop net he had set up above the garbage can in his office. However, in this case, the tumor and resection also partly involved the superior portion of area 7.
Others neurons in area 5 are especially responsive to particular temporal-sequential patterns of sensation (LaMotte & Mountcastel, 1979) and can determine direction and rhythm of movement. It is presumably through the activity of these cells that one can "hear" via the detection of vibrations (such as reported by the deaf). In fact, auditory as well as visual simulation can induce activation of this region (Lam et al., 1999).
THE BODY IN SPACE
Signals from joint and cutaneous receptors are transmitted to association neurons (Skata & Iwanura 1978). Many associaton cells also receive converging input from primary neurons concerned with different body parts (Dong et al. 2014; Sakata, et al. 2015), and can combine these signals with visual information (Snyder et al., 1998) and are thus able to determine positional interrelationships.
For example, a single association neuron may receive information regarding the elbow and the shoulder, and become activated only when these two body parts are simultaneously stimulated or in motion. A considerable number of cells are especially sensitive to the posture and position of the trunk and extremities during movement (Hyvarienen, 1982). By associating this convergent input these cells are thus able to monitor, coordinate and guide limb movement (Cohen et al. 2014) as well as determine the position of the body and objects in space.
Through the integrative and associative activities of the cell assemblies within area five, an interactional image of the body is maintained. In this manner, an individual is able to ascertain the positon of the body and the limbs at rest and in motion (Gross, et al. 1974). In part, this may be accomplished through comparisons with a more stable image of the body which is possibly maintained via the combined interactions of neurons in areas 3,1,2. That is a stable body image (or body image memories) are stored in these tissues. Hence, when the body has moved, this new information (received and processed in area 5) can be compared to the more stable trace (or memory maintained in the primary regions) so that the new position of the limbs and body can be ascertained. In this regard it could be argued that body-related memories are stored in the parietal lobe.
Nevertheless, to determine position, sensation per se is not sufficient. Rather, sensation must be combined with input regarding movement or positional change (Gandevia & Burke 1992). It is for this reason that in the absence of movement (and in the absence of visual cues, such as when one wakes up in the middle of the night) one usually cannot tell where or in what position their arms or legs may be in. However, with a slight movement we can immediately determine position.
TACTILE DISCRIMINATION DEFICITS & STEREOGNOSIS
Massive destruction of the somesthetic association area results in many of the same disturbances which occur following lesions of the primary region. This includes abnormalities involving two-point discrimination, position sense, and pressure sensitivity. However, detection threshold is not altered (LaMotte & Mountcastle, 1979). For example, a patient may recognize touch, but be unable to localize what part of the body has been stimulated.
For example, following a right parietal stroke one patient made gross errors of localization when I touched various regions of his body while his eyes were closed. For example, he named his elbow when I touch his leg, and his shoulder when his wrist was touched. He in fact expressed considerable astonishment when I allowed him to open his eyes after each test so as to see where the stimulation was actually being applied.
In addition, with destruction of this tissue, although a patient may be able to recognize that he is holding something in his hand he may be unable to determine what it might be (astereognosis). In these later instances, however, the cortical area representing the hand must be compromised.
With small lesions involving only a particular part of the somesthetic cortex (e.g. the area representing the arm and shoulder), the deficit will be only manifested when the part of the body represented is examined. For example, the patient may be able to localize touch and determine the direction of a moving stimulus when it is applied to the hand, face, or leg, but be unable to do so along the shoulder or arm if this area of the cortex has been compromised.
The laterality of the lesion is also important, right sided damage having more drastic effects on somesthesis and stereognostic functioning than left parietal lesions. In addition, although lesions to either parietal lobe can give rise to astereognosis (an inability to recognize objects tactually explored), lesions to the right parietal lobe are likely to give rise to bilateral abnormalities, whereas left parietal injuries generally effect only the right hand (Hom & Reitan, 1982). Again, however, astereognostic deficits require that the somesthetic area representing the hand (see below) be comprised (Roland, 1976).
Larger lesions extending into the posterior parietal lobe, area 7, also decrease the ability to perform size, roughness, weight and shape discriminations (Blum, Chow & Pribram, 1950; Denny-Brown & Chambers, 1958; Garchas et al., 1982; Ridley & Ettlinger, 2015; Semmes & Turner, 1977).
REFERENCES












