Rhawn Gabriel Joseph, Ph.D.
BrainMind.com
Schizophrenia is a disorder of emotion, thought, and language. Schizophrenics, in the acute (initial) phase of their illness may display a flatness of emotion which then flares up into exceedingly brief and sometimes prolonged rages, depressions, or mania. Thinking is disordered, and speech may become silly, nonsensical, or bizarre, and sprinkled with neologisms, clang associations, and paraphasias.
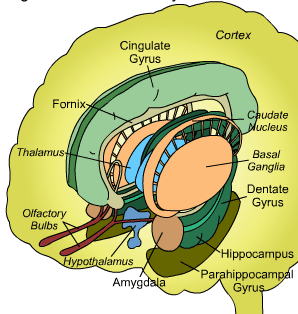
Schizophrenia is associated with abnormalities of the frontal and temporal lobes, as well as the basal ganglia (caudate) and amygdala.
Schizophrenia has been associated with the left temporal lobe as measured by positron-emission tomography (e.g. McGuire et al. 2012), P300 evoked potential amplitude (Bruder et al., 2016; Salisbury et al. 2012) and MRI (Jacobsen et al. 2012; Shidhabuddin et al. 2013; Kwon et al., 2015).
Schizophrenia has also been associated with the left frontal lobe (Joseph, 2015a). Reductions in left frontal gray matter and brain volume reductions and decreased activity have been repeatedly noted, including decreased blood flow, hypoactivity, and reduced metabolism (Arieal et al. 1983; Berman et al. 1986; Buchsbaum et al. 1992; Ingvar, & franzen, 1974; Weinberger, et al. 1986).
Moreover, pathological abnormalities have been found in the amygdala, hippocampus and hypothalamus, and lateral ventricules.
SCHIZOPHRENIA
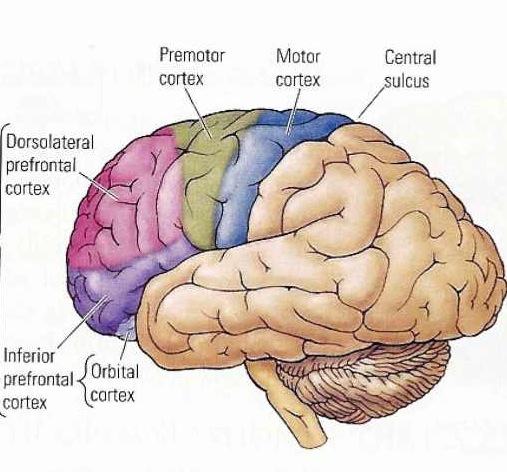
A variety of anatomical as well as biochemical disturbances have been found in various populations of individuals diagnosed as suffering from "schizophrenia" (Akbarian et al. 1993; Benes, 2005; Buchanan et al. 2007; Buchanan et al. 2012; Bruton et al. 2007; Curtis et al. 2012; Stanely et al. 2005). These disturbances include impaired interhemispheric transfer of visual, auditory and somesthestic information (Beaumont & Dimond, 1973; Carr, 2003; Green & Kotenko, 2004), increased lateral ventricular size (Berman et al. 1987; DeQuardo et al. 2007), increased corpus callosum thickness (Rosenthal & Bigelow, 1972), pathological abnormalities in the temporal lobes, amygdala, hippocampus and hypothalamus (Akbarian et al. 1993; Benes, 2005; Berman et al., 1987; Brown et al., 1986; Bogerts et al. 1985; Crowe & Kuttner 1991), reduced prefrontal cortical metabolic activity (Arieal et al., 1983; Berman et al. 1986; Ingvar, & franzen, 1974; Weinberger, et al. 1986), medial frontal lobe dysfunction (Joseph 2010d, see chapter 11), dorsolateral frontal abnormalities (Akbarian et al. 2005; Stanley et al. 2005), and disturbances involving the basal ganglia and dopamine neurotransmitter system (Swerdlow & Koob, 1987; see chapter 16).
In part, the reason so many different brain areas are implicated is secondary to the wide range of symptoms that various researchers and physicians may diagnose as "schizophrenic" (e.g. Andreasen et al. 2005). Indeed, as is well known (at least among psychiatrists) a perusal of most any patients diagnostic history will often reveal a variety of diagnoses that appear to change as frequently as the patient changes doctors (DSM's I-IV not withstanding).
Nevertheless, in the majority of studies that has addressed the issue of laterality, localization, and "schizophrenia", left frontal and in particular left temporal lobe abnormalities have been reported (e.g. Abrams & Taylor, 2003; Flor-Henry, 1983; Morihisa et al. 1983; Morstyn, et al. 1983b; Trimble 1991). These abnormalities include left lateral frontal gray matter and brain volume reductions and decreased activity, decreased blood flow, and reduced metabolism (Arieal et al. 1983; Berman et al. 1986; Buchsbaum et al. 1992; Ingvar, & franzen, 1974; Weinberger, et al. 1986). Although bilateral frontal and temporal lobe abnormalities have been observed (Bruton et al. 2007), unilateral dysfunction of the right half of the brain has not been demonstrated as significantly related to the manifestations of these disturbances.
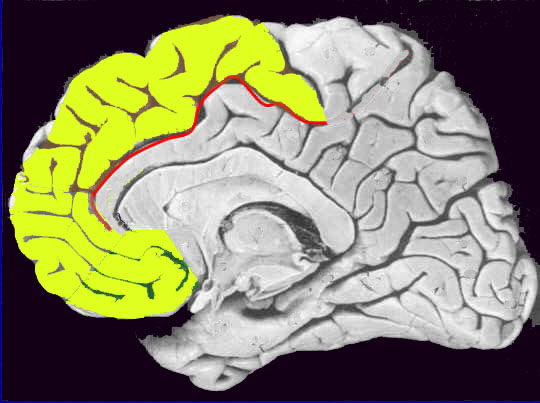
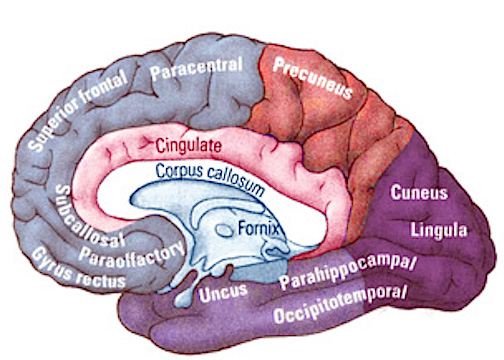
Thus, abnormalities predominantly involving the left hemisphere and the left frontal and temporal lobe are indicated in a sizable minority of patients diagnosed with schizophrenia, with the single exception that so called "catatonic-schizophrenia" is predominantly (if not exclusively) associated with medial frontal lobe damage (Joseph 2015a) and related to dysfunction involving the head of the caudate and perhaps, indirectly, the amygdala.
FRONTAL LOBE SCHIZOPHRENIA
Individuals classified as schizophrenic demonstrate EEG and other abnormalities suggestive of bilateral or left frontal dysfunction or hypoarousal (Akbarian et al. 1993, 2005; Ariel et al. 1983; Buchanan et al. 2012; Curtis et al. 2012; Ingvar & Franzen, 1974ab; Kolb & Whishaw, 1983; Levin, 1984; Stanley et al. 2005). Schizophrenic patients who are most likely to be suffering from frontal lobe dysfunction tend to display unusual mannerisms, catatonia, "emotional blunting", apathy, and/or "Hebephrenia" (puerile, silly, childish, disinhibited and jocular behavior), though negative symptoms predominate. Indeed, almost 50 years ago Hillbom (1951), reported a strong association between individuals with head trauma and missle wounds to the frontal lobe who later developed schizophrenic-like symptoms, including catatonia and hebrephrenia if the medial or right frontal lobes are also impacted.
As detailed in chapter 19, if the medial frontal lobes are damaged or experimentally electrically stimulated, there sometimes results in a inability to initiate a voluntary movement, and the "Will" to move or speak may be completely attenuated and abolished (Hasslet, 2003; Laplane et al. 1977; Luria, 2003; Penfield & Jasper, 1954; Penfield & Welch, 1951). Similarly, lesions of the medial frontal lobes can cause subjects to simply sit or stand motionaless, as if frozen, and display waxy flexibility, or "gegenhalten" or counterpull -- i.e. involuntary resistance to movement of the extemities (Brutkowski, 1965; Hasslet, 2003; Laplane et al., 1977; Luria, 2003; Mishkin, 1964). Posturing is also noted and patients might remain in odd and uncomfortable positions for exceedingly long time periods and make no effort to correct the situation (Freeman & Watts, 1942; Rose, 1950), as if they were dead and in the first stages of rigor mortise. These are all classic signs of catatonia.
By contrast, apathetic, blunted, and "negative" forms of schizophrenia coupled with "psych-motor retardation" reduced verbal and intellectual output and slowness of thought, tend to be associated with the left frontal lobe dysfunction (Buchsbaum, 2010; Carpenter et al. 1993; Casanova et al. 1992; Crow & Kuttner, 1991; Leven 2007; Stanley et al. 2005; Weinberger 1987). Nevertheless, because of the apathy and reduced speech and motor output, these patients may variably be diagnosed as depressed.
LATERAL FRONTAL PSYCHOSIS, & NEOCORTICAL INFORMATION PROCESSING
A variety of studies which have implicated the lateral frontal lobes in the genesis of certain forms of schizophrenia (Akbarian et al. 1993, 2005; Buchsbaum, 2010; Buchanan et al. 2012;Carpenter et al. 1993; Casanova et al. 1992; Curtis et al. 2012; Crow & Kuttner, 1991; Leven 2007; Stanley et al. 2005; Weinberger 1987). As detailed in chapter 19, the lateral frontal lobes receive converging sensory input from the primary, secondary, and association areas for audition, vision, and somesthesis. In addition, whereas the orbital frontal lobes regulate subcortical and limbic arousal, the lateral frontal lobes, via massive interconnections with the dorsal medial thalamus and the posterior neocortex, is able to regulate neocortical information processing and arousal.
However, in addition to frontal lobe hypoactivity, dysfunction, and studies indicating a reduction in dendritic spines, synapses, and cortical neuropil, it has been reported that the thalamus is diminished in size. Specifically, a reduction in dorsomedial thalamic neurons has been reported (see Lewis 2005).
As detailed in chapter 19, disruptions of the integrity of the lateral frontal-thalamic-neocortical regulatory circuit can result in sensory overload, confusion, disorientation, memory loss, thereby creating profound psychological and cognitive disturbances which may be manifested as psychosis, thought blocking, psychomotor retardation, etc. Conditions such as these, however, may also be induced by frontal lobe hypoactivity and or disturbances in the frontal GABA neurotransmitter system (Akbarian et al. 2005; Benes, 2005; Lee & Tobin 2005). GABA is an extremely potent inhibitor of neural activity. Reductions in GABA could result in neocortical disinhibition and thus sensory overload, confusion, and psychosis.
In this regard it is noteworthy that Akbarian and colleagues (2005), have presented evidence which suggests that the genesis for frontal lobe hypoactivity in schizophrenics is due to cellular abnormalities in the level of messenger RNA for glutamac acid decarboxylase (GAD). GAD is normally present in about 30% of lateral frontal neurons, particularly those which rely on GABA as a neurotransmitter.
As pointed out by Lee and Tobin (2005), decreases in frontal lobe GABA could well result in compensatory increases in GABA receptors in the caudate, temporal lobe and cingulate, which have also been demonstrated in patients with schizophrenia. However, GABA overactivity in the caudate, and in particular the temporal lobe is associated with positive symptoms, whereas negative symptoms are linked to the lateral frontal lobe, which suggests these regional differences in GABA activity may not be necessarily linked.
.
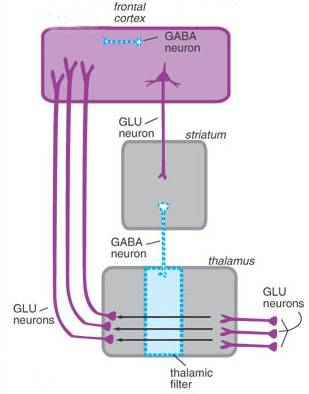
Perhaps more importantly, lateral frontal GABA neurons receive significant input from DA axons. About 30% of frontal DA axons terminate on GABA dendrites which also receive DA input from the striatum (see chapters 6 & 8). In consequence, GABA abnormalities can induce DA abnormalities within the frontal lobe as well as within the basal ganglia.
STRIATAL SCHIZOPHRENIA
It is likely, as in obsessive-compulsive disorders, that schizophrenic-like abnormalities associated with the frontal lobe may in fact be due to disruption of the basal ganglia-DA-medial/lateral frontal circuit. In this regard, as the extent of caudate-DA involvement increases, so too does the severity of schizophrenia. As is well known, many of the major antipsychotic drugs act on dopamine receptors within these nuclei.
In primates and humans, lesions, destruction, or shrinkage of the head of the caudate can result in sensory neglect, agitation, hyperactivity, and in some cases what appears to be a manic or "schizo-affective" psychosis (Aylward et al. 2007; Caplan, et al. 2010; Castellanos et al. 2007; Chakos et al. 2007; Davis, 1958; Richfield, et al. 1987) depending on the extent and laterality of the destruction.
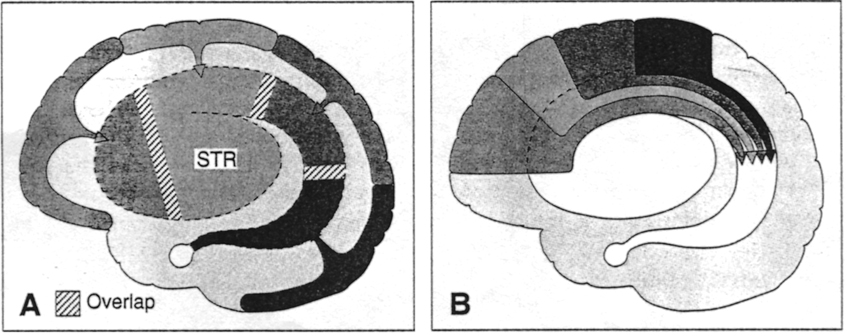
Some patients will alternate between and/or display a variable mixture of hyperactivity and schizophrenic-like apathy, depending, in part, on the laterality and extent of the lesion as well as associated biochemical alterations. For example, injuries or abnormalities restricted to the right caudate are more likely to result in a manic-like psychosis (Castellanos et al. 2007) --quite similar to what occurs after right frontal lobe injury (Joseph 1986a, 1988a, 2015a)- whereas left caudate lesions tend to mimic left and medial frontal dysfunction.
For example, with extensive left or bilateral caudate injuries it is not uncommon for patients to appear agitated, apathetic, with decreased spontaneous activity and slowed and delayed, dysarthric (or stuttering) and emotionally flat speech, with some patients responding to questions only after a 20-30 second delay (Caplan et al. 2010). This condition is particularly likely if the medial frontal lobes have been compromised as well.
MEDIAL FRONTAL/STRIATAL CATATONIA
Due perhaps to its extensive interconnections with the medial frontal lobes and the supplementary motor areas (SMA) -a region which when destroyed can give rise to catatonia (Joseph 2015a), massive bilateral lesions to the anterior caudate and anterior putamen and surrounding tissue has been shown to produce catatonic or "frozen" states, where animals show a tendency to maintain a single posture or simply stand unmoving for weeks at a time (Denny-Brown, 1962).
Similarly, chemically lesions of the caudate can produce complete catatonia, posturing and a cessation of all movement (Spiegel & Szekely, 1961). Conversely, because benzodiazipine receptors are located throughout the striatum, anti-psychotic agent, due to their dopamine properties, can reduce this abnormal activation and reduce catatonic, schizophrenic, as well as related psychotic disturbances of thought and behavior.
DOPAMINE & THE CAUDATE
A major function of the head of the caudate (particularly the caudate nucleus of the right hemisphere) appears to be inhibition. Similarly, the principle effect of striatal DA is inhibition (Ellison, 2007; Le Moal & Simon 1991; Mercuri, et al. 1985). In consequence, excessive and abnormal amounts of corpus striatal DA can result in increased levels of caudate-putamen activity such that limbic striatal, and the reception of amygdaloid/emotional input into the striatum may be severely diminished and/or abnormally processed, thereby producing confusion and cognitive-emotional disorganization.
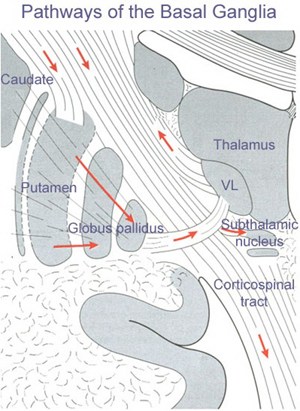
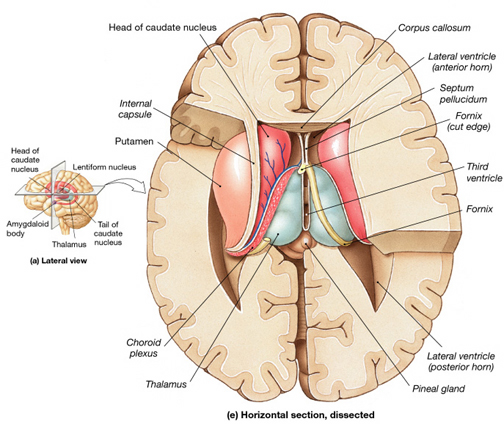
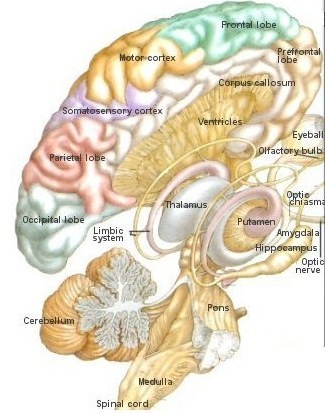
Similarly, individuals diagnosed as paranoid and schizophrenic with psychomotor retardation have been found to have elevated DA levels and increased DA receptor binding (Crow, 1979; Ellison, 2007; Matthyse, 1981; Ring et al. 2007). Therefore it appears that excessive corpus striatal activity and with increases in striatal DA, can induce massive inhibition and emotional blunting or distortion as well as cognitive abnormalities such that effected individuals appear psychotic (see Castellanos et al. 2007; Chakos et al. 2007; Ring et al. 2007; Snyder, 1972).
Conversely, because benzodiazipine receptors are located throughout the striatum, anti-psychotic agents, due to their dopamine properties, can reduce this abnormal activation. Presumably this is why dopamine blockers such as the phenothiazines are effective in reducing psychotic behavior; i.e. they reduce excessive DA binding and excessive striatal activity which in turn restores the capability of the striatum (and related nuclei) to engage in cognitive-emotional integrative and related analytical activities.
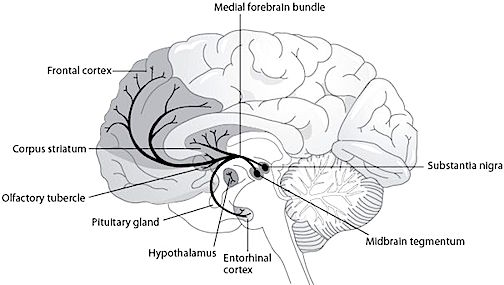
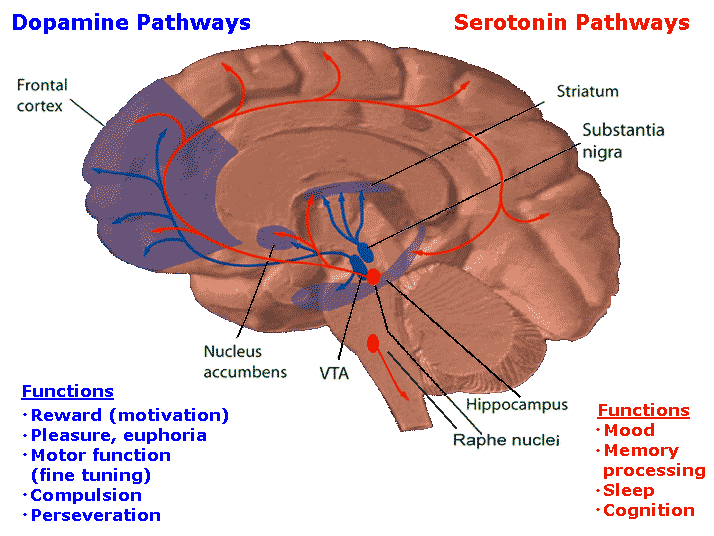
TEMPORAL LOBE SCHIZOPHRENIA
Psychotic disturbances, including "schizophrenia" need not involve the frontal lobe, basal ganglia or DA dysfunction, as disorders of thought and mood may also appear following temporal lobe damage. For example, it has been repeatedly reported that a significant minority of individuals with temporal lobe epilepsy suffer from prolonged and/or repeated instances of major psychopathology (Bruton et al. 2007; Buchsbaum, 2010; Flor-Henry 1969; Perez & Trimble 2003; Slater & beard, 1963; Taylor 1975; Umbricht et al. 2005). These estimates range from 3% to 7% (see Trimble, 1991, 1992). Moreover, schizophrenia has been associated with the left temporal lobe as measured by positron-emission tomography (e.g. McGuire et al. 2012), P300 evoked potential amplitude (Bruder et al., 2015; Salisbury et al. 2012) and MRI (Jacobsen et al. 2012; Shidhabuddin et al. 2012; Kwon et al., 2015). Moreover, pathological abnormalities have been found in subcortical temporal lobe structures, i.e., the amygdala and hippocampus (Akabarian et al. 1993; Berman et al., 1987; Brown et al., 1986; Bogerts et al. 1985; Crowe & Kuttner 1991), as well as the lateral ventricules (Berman et al. 1987; DeQuardo et al. 2007).
Similarly, it has been repeatedly demonstrated in histological studies that the temporal lobe of schizophrenics are characterized by an excessive focal temporal lobe neuronal damage including gliosis as well as evidence of neural migration errors (Akbarian et al. 1993; Bruton 1988; Bruton et al. 2010; Stevens 1982; Taylor 1972). This includes volume reductions in the left anterior portions of the amygdala and hippocampus, parahippocampal gyrus, and superior temporal lobe; abnormalities in the orientation of and decreases in the humber of hippocampal neurons; as demonstrated by postmortem and MR imaging studies (e.g. Trojanowski & Arnold 2005; Wible et al. 2005).
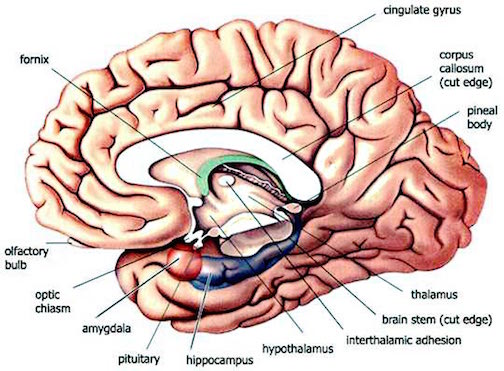
"Schizophrenia" associated with the left temporal lobe, however, is markedly different from that manifested by left frontal, medial frontal, or basal ganglia lesions. For example, individuals with medial frontal lobe "schizophrenic" dysfunction are more likely to demonstrate thought blocking, sever apathy, catatonic symptoms as well as mutism. Those with left frontal dysfunction may demonstrate poverty of speech, reduced motor activity, apathy, as well as depressive and blunted forms of schizophrenia. Those with basal ganglia involvement may present with a mixture of frontal and temporal lobe signs (see chapters 4, 9 & 11).
However, in contrast to the "negative" symptoms associated with frontal lobe schizophrenia, temporal lobe schziophrenics are likely to present with "positive" symptoms, incuding the capacity to experience and express "warmth" (Crow, 2003; Crowe & Kuttner 1991; Wible et al. 2005). Patients with schizophrenia who display "positive" symptoms tend to display temporal lobe but not frontal lobe abnormalities (Wible et al. 2005).
Emotional expression in temporal lobe schizophrenics, however, tends to be highly abnormal, inappropriate, incongruent, and/or exaggerated (Bear & Fedio, 1977; Crow, 2003; Crowe & Kuttner 1991). It is also not uncommon for these individuals to demonstrate aphasic abnormalities in their thought and speech (Chaika, 1982; Clark et al. 2007; Flor-Henry, 1983; Hoffman, 1986; Hoffman et al. 1986; Perez & Trimble, 2003; Rutter, 1979; Slater & Beard, 1963) as well as to develop severe paranoid and related affective abnormalities, including auditory as well as visual hallucinations -particularly if the anterior-inferior temporal lobe and the amygdala and hippocampus are involved (Bogerts et al. 1985; Brown et al. 1986; Falkai & Bogerts 1986) -in which case memory may also be effected.
Temporal lobe schizophrenics with limbic involvement may also behave violently and aggressively (Crow & Kuttner 1991; Lewis et al. 1982; Taylor 1969). They may also experience extreme feelings of religiousness (Bear, 1979, Trimble, 1991, 1992), fear, and paranoia, and depression (Crow & Kuttner 1991; Perez & Trimble, 2003; Trimble, 1991, 1992) as well as auditory and visual hallucinations ranging from angry accusatory voices from disembodied spirits, dead relatives, to frightening images of ghosts, demons, angels, and even God, as well as sensations of demonic and angelic possession (Bear 1979; Daly 1958; Gloor 1986, 1992; Horowitz et al. 2018; MacLean 1990; Mesulam 1981; Penfield & Perot 1963; Schenk, & Bear 1981; Slater & Beard 1963; Subirana & Oller-Daurelia, 1953; Trimble 1991; Weingarten, et al. 2017; Williams 2016).
THE AMYGDALA, DA & SCHIZOPHRENIA
In some instances of schizophrenia, the frontal lobe, basal ganglia and DA transmitter systems are often effected (see chapters 16 & 17). However, the amygdala is also a major part of the basal ganglia and it is also significantly influenced by DA. Indeed, abnormal DA as well as norepinephrine (NE) and serotonin (5HT) have been reported in the amygdala of those diagnosed as psychotic (Spoont 1993; Stevens 2012).
However, a gross asymmetry in the post-mortem levels of mesolimbic DA has been noted in the brains of those diagnosed as schizophrenic (Le Moal & Simon 1991). Specifically, an increase in DA has been noted in the central amygdala and in the striatum of the left hemisphere, whereas DA levels within the right cerebral are similar to normals.
In fact, the left amygdala and left temporal lobe (Flor-Henry, 1969; Perez, et al. 1985; Stevens, 1992) have long been thought to be a major component in the pathophysiology of psychosis and schizophrenia (Heath, 1954; Stevens, 1973; Torey & Peterson, 1974). For example, abnormal activity as well as size decrements have been noted in the left amygdala (Flor-Henry, 1969; Perez, et al. 1985) as well as the left inferior temporal lobe in schizophrenic patients (see Stevens, 1992). Spiking has also been observed in the amygdala of psychotic individuals who are experiencing emotional and psychological stress (see Halgren, 1992).
In this regard it has been suggested that stress, particularly when experienced prenatally may be responsible, in some cases, for the development of DA abnormalities (see Le Moal & Simon 1991), whereas adverse early environmental experiences and trauma may contribute to the development of kindling, spiking and abnormal amygdala functioning (see chapter 16).
APHASIC & PSYCHOTIC SPEECH
Given that Wernicke's receptive speech area is located within the left temporal lobe, afflicted individuals may experience auditory hallucinations and are more likely to demonstrate formal thought disorders and aphasic thinking including the production of neologisms and syntactical speech errors, as well as emotional (or thought) blocking or blunting due to limbic system-temporal lobe disconnection (Perez & Trimble, 2003; Slater & Beard, 1963). As often occurs with receptive aphasia and left temporal lobe dysfunction, individuals suffering from schizphrenia may be unaware of their illness (Amador et al. 2007; Wilson et al. 1986).
Hence, certain subgroups of schizophrenics display significant abnormalities involving speech processing, such that the semantic, temporal-sequential, and lexical aspects of speech organization and comprehension are disturbed and deviantly constructed (Chaika, 1982; Clark et al. 2007; Flor-Henry, 1983; Hoffman, 2016; Hoffman et al. 2014; Rutter, 2009). Indeed, significant similarities between schizophrenic discourse and aphasic abnormalties have been reported (Faber et al. 1983). Moreover, it has been reported that the severity of the thought disorder is directly related to abnormalities in the asymmetry of the planum temporale (Petty et al. 2005).
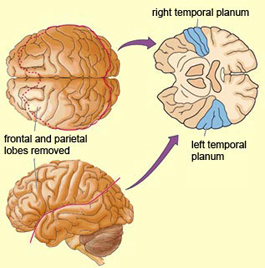
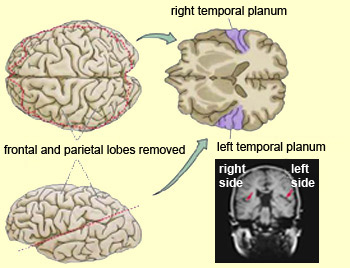
Conversely, because individuals with Wernicke's aphasia display unusual speech, loss of comprehension, a failure to comprehend that they no longer comprehend or "make sense" when speaking, as well as paranoia and/or euphoria, they are at risk for being misdiagnosed as psychotic or suffering from a formal thought disorder, i.e. "schizophenia".
Hence, there is considerable evidence indicating that a a significant relationship exists between abnormal left hemisphere and left temporal lobe functioning and schizophrenic language, thought and behavior (see also chapters 14 & 17).
BETWEEN SEIZURE PSYCHOSES
Estimates of psychosis and affective disorders among individuals suffering from temporal lobe epilepsy, be it a single episode or chronic psychiatric condition have varied from 2-81% (Falconer, 1973; Flor-Henry, 1983; Gibbs, 1951; Jensen & Larsen, 1979; Sherwin, 1977, 1981; Taylor, 1972; Trimble 1991). Probably a more realistic figure is about 4.5 to 7% (Trimble 1991).
Frequently these disturbances wax and wane, such that some patients experience islands of normality followed by islands of psychosis (e.g. Flor-Henry 1983; Umbricht et al. 2005). Possibly these changes are a function in variations in subclinical seizure activity and kindling.
In some instances, the psychiatric disturbance may develop over days as a prelude to the actual onset of a seizure, due presumably to increasing levels of abnormal activity until the seizure is triggered. In other cases, the alterations in personality and emotionality may occur following the seizure and may persist for weeks or even months (Trimble 1991; Umbricht et al. 2005).
In yet other instances, patients may act increasingly bizzare for weeks, experience a seizure, and then behave in a normal fashion for some time ("forced normalization", Flor-Henry 1983), only to again begin acting increasingly bizzarre (Umbricht et al. 2005). This has been referred to as an inter-ictal (between seizure) and postictal psychosis and is possibly secondary to a build up of abnormal activity in the temporal lobes and limbic system (Bear, 1979; Flor-Henry 1969, 1983) Hence, once the seizure occurs, the level of abnormal activity is decreased and the psychosis goes away only to gradually return as abnormal activity again builds up.
CONGENITAL & EARLY ENVIRONMENTAL CONTRIBUTIONS TO SCHIZOPHRENIA.
The brain is susceptible to a variety of disruptive and damaging influences including emotional trauma and stress, stroke, tumors, seizures, degenerative and biochemical abnormalities, drugs, alcohol, toxic exposure, and congenital trauma and related abnormalities.
However, the nature of the disruption, and the areas of the brain most effected, are determined not just by the causative agents but also by the timing. For example, prenatal disturbances of early onset (e.g. a viral infection) may selectively interfere with neural migration and thus cortical formation, whereas an identical disturbance experienced just prior to birth may have little or no effect on brain development.
As noted, be it a prenatal infection or a trauma, or a cerebral infarct suffered at age 60, in general it is only the more moderate to severe disturbances which are likely to come to the attention of the physician. However, as to mild abnormalities, such as a small and circumscribed stroke, there is the possibility that related deficits may go unnoticed by friend, family, and even the patient himself.
The same is true regarding prenatal damage, the effects of which may not become fully manifest until later in life; at which point the symptoms may be mistakenly assumed as having their onset at this later time period. Disturbances of prenatal origin but adult onset includes abnormalities referred to as "schizophrenia" as well as a host of related and unrelated disabilities involving intellect, cognition, and emotional functioning (e.g. Akbarian et al. 1993, 2005; Benes, 1991, 2005; Lewis 2005).
Consider, for example, the broad symptom complex that is associated with "schizophrenia." As detailed in previous chapters, a variety of anatomical as well as biochemical disturbances have been found in various populations of individuals diagnosed as suffering from this disorder. Although these abnormalities in some cases are due to infarcts, tumors, and degenerative disturbances experienced as an adult, they may just as likely be congenital and secondary to intrinsic and extrinsic prenatal influences which result in neuronal migration errors, abnormal synaptic interconnections, increased ventricular size, basal ganglia and cerebellar abnormalities, and so on.
As noted above, Akbarian and colleagues (2005) have demonstrated that the frontal lobes of individuals diagnosed as schizophrenic show a reduced expression of glutamic acid decarboxylase (GAD), which is a key enzyme in GABA synthesis. Presumably, reduced GAD expression is linked to or brought about by reduced frontal lobe activity (Akbarian et al. 2005). However, Akbarian and colleagues (2005) also argue, based on their studies, since they failed to find any alterations in actual cell numbers, that this condition may not be due to disturbances in neural migration per se.
On the other hand, Akbarian et al. (1993) have reported that a small population of nicotineamide-adenine dinucleotide phosphate-diaphorase neurons located in the white matter of the frontal and temporal lobes, are also abnormal in schizophrenics; disturbance which appear to be directly linked to cogenital abnormalities in cerebral development. Coupled with their 2005 data, Akbarian and colleagues (2005) suggest therefore, that these conditions (i.e. reduced GAD, altered neuronal distribution in the white matter) may well be due to disturbances of neuronal migration or abnormalities involving the cortical subplate during early embryonic formation of the brain. Because the cortical subplate serves as the terminal junction for migrating neocortical neurons (see chapter 18), abnormalities involving the subplate may in turn result in white matter abnormalities and diplaced (subplate) neurons, as well as reduced GAD expression within all six layers of the neocortex of schizophrenics (see also Lewis 2005).
In addition, reductions in layer II and III interneurons have been reported in the brains of schizophrenics (reviewed in Benes 2005). An increase in synaptic interconnections between layer I and II has also been documented (Benes 2005). Normally these initial interconnections (which serve to nourish and maintain the cell until its true synaptic counterpart is available) drop out as surrounding neurons and those which are still arriving, begin to differentiate, mature, and grow axons and dendrites (see chapter 18). Presumably, layer I neurons maintains these interconnections due to the failure of their normal counterparts to successfully complete their migration (thus creating white matter heterotopias).
A neurodevelopmental disturbances involving select aspects of neural migration or cortical formation would also explain the lack of gliosis. That is, these and other indications of preferential tissue or neurochemical loss in the absence of gliosis argues against a degenerative process of late onset -at least in these cases.
Hence, in some instances, individuals suffering diagnosed as suffering from schizophrenia may well have suffered a prenatal insult to the brain; e.g. viral infection, malnutrition (see chapter 18) which resulted in migration errors, abnormal neuronal distribution and displacement, and thus neocortical as well as white matter abberations.
ABUSE & CEREBRAL DEVELOPMEN.
Cerebral development continues well past the first decade (chapter 18). Indeed, for the first few years of life large regions of the neocortex are markedly immature, and this includes the frontal and temporal lobe, and in fact, layers II and III of the neocortex -layers which contain local circuit neurons which interlink various neocortical areas. As neurons are still maturing, and as dendritic and axonal synaptic connections are still being formed, the brain of the child, like that of the neonate, is also at risk for developing abnormally.
Psychotic individuals often have children who are reared in a psychotic environment. Many children are also neglected and physically and sexually abused by seemingly "normal" parents (chapter 28, 20). Babies may be shaken repeatedly, inducing axonal and neocortical shearing as well as coup and contra coupe lesions, and they may be battered, struck in the head, or held by the legs as parents or caretakers, siblings, etc., slam them against walls or furniture. Unless life threatening, children who are abused do not always come to the attention of the authorities. Those who are emotionally abused, rarely so.
Nevertheless, and as detailed in chapters 23-29, because different regions of the brain take years if not decades to completely mature, and due to the plastic capabilities of the immature cerebrum, severe emotional and environmental stress, be it neglect or physical abuse, can induce structural abnormalities in the brain, the temporal lobes in particular, as well as create and establish abnormal neural interconnections. Indeed, the brain of a young child is particularly susceptible to repetitive and severe emotional stress, as well as stroke or head injury; all of which can induce significant brain damage and functional/structural abnormalities.
In addition, when these emotional stresses are coupled with the abnormal learning that characterizes abusive parent-child relationships and early rearing experiences associated abnormal neural networks are created and abnormal emotional, cognitive, and behavioral functioning results (Joseph 1992b). However, depending on the age of the child and even the type of stress or abuse (e.g. nutritional) different regions of the brain may be effected to different degrees.
SCHIZOPHRENIA, EARLY ONSET FRONTAL LOBE INJURY & SYMPTOM FORMATION.
Although "schizophrenia" seems to develop in the late teens, early twenties and beyond, as indicated above, the disturbance may well be congenital in origin and/or due to early childhood emotional or physical trauma. However, if congenital or due to childhood trauma, why the long delay in the development of psychotic symptoms? Moreover, when considering, for example, the role of the frontal lobes in attention, arousal, inhibition, etc., or the temporal lobes in memory, it would seem that if these regions became abnormal early in life, or congenitally, that related abnormalities would become immediately apparent.
Possibly, as has been demonstrated with primates, frontal dysfunction of early onset, does not become fully manifest until later in life (e.g. Goldman-Rakic, 1974); that is, when the frontal lobes are required to assume new functions. Similarly, the temporal lobe, the inferior regions in particular, continue to develop and mature well into late childhood and beyond (Blinkov & Glezer 1968; Conel 1937-1963).
On the other hand, it has also been demonstrated that some children suffering from autism (which has also been referred to as childhood schizophrenia) suffer from maturational delays involving the frontal cortex (Zibovicious et al. 2005). In these instances, related psychological abnormalities are apparent often within the first two years of life.
Possibly, at least in cases of congenital or early childhood origin, what appears to be adult vs childhood onset is really a matter of degree. That is, those who are most severely effected demonstrate severe psychotic symptoms which are recognized at an earlier age, whereas those who are mild to moderately abnormal are able to better manage and cope. Nevertheless, in this regard it is noteworthy that many adults diagnosed as schizophrenic were often viewed by school mates and teachers, if not by their parents as odd, socially inept or withdrawn, even as children. However, although "odd" (and probably psychotic) as these "pre-schizophrenic" children are still cared for by parents and spend much of their time alone in a structured environment (school), the full range of their pathology is not always evident.
However, once these individuals leave the structured environment provided by school (including college) and are expected to fend for themselves, it is not uncommon for their problems to finally come to the attention of the authorities, social workers, psychologists and psychiatrists. This is particularly true of males (e.g. Szymanski et al. 2005) who are expected to become independent at an earlier age and who are far less likely, once they reach adulthood, to find someone to take care of them. By contrast, even psychotic females may be able to trade sexual favors so as to get married and/or have someone provide for them. Thus, a consistent finding is that males are hospitalized at an earlier age, have more frequent hospitalizations with longer stays, and suffer more frequent relapses (e.g. Szymanski et al. 2005). Of course, sex differences in cerebral functioning are probably also contributory. In this regard it is noteworthy that young males appear to be more vulnerable to early environmental trauma, particularly emotional neglect and they are not as resilient and do not appear to recover as much or as quickly as females after removal from these environments.
CONCLUSION
Although encased in a thick skull, covered by leathery tough meninges, and protected by a blood-brain barrier, the brain is subject to a myriad of environmental and intrinsic insults, beginning soon after conception, and continuing until death. Often it is only when the brain damage is moderate to severe, or involves speech and the motor system, that medical or psychological treatment may be sought.
The same is true regarding prenatal lesions. Moreover, unless moderate to severe, subsequent cognitive, intellectual, and emotional abnormalities due to congenital or early environmentally induced lesions may not become manifest until later in life. In fact, even after these related disturbances become manifest, the underlying neurological foundations may be completely overlooked.
The same is true regarding adults. It is not uncommon for patients to suffer from, for example, an expanding medial frontal tumor, and to be diagnosed as depressed, but for the tumor to be overlooked. Or, to suffer scrotal pain or electric shock-like sensations, due to a parietal tumor, but to be viewed as hysterical. Nevertheless, be it congenital abnormalities, small infarcts, neoplasm, slowly progressive deteriorative or biochemical disorders, subclinical seizures, early environmental emotional trauma, or even "mild" head injuries, these insults are often the triggering event if not the root cause of many if not most psychotic and related cognitive and emotional disorders. The symptom complex, however, is dependent not only on the nature of the disturbance (e.g. tumor, neurotransmitter) but the location (e.g. frontal vs temporal) and the timing of the original intrinsic insult or environmental/emotional trauma.












